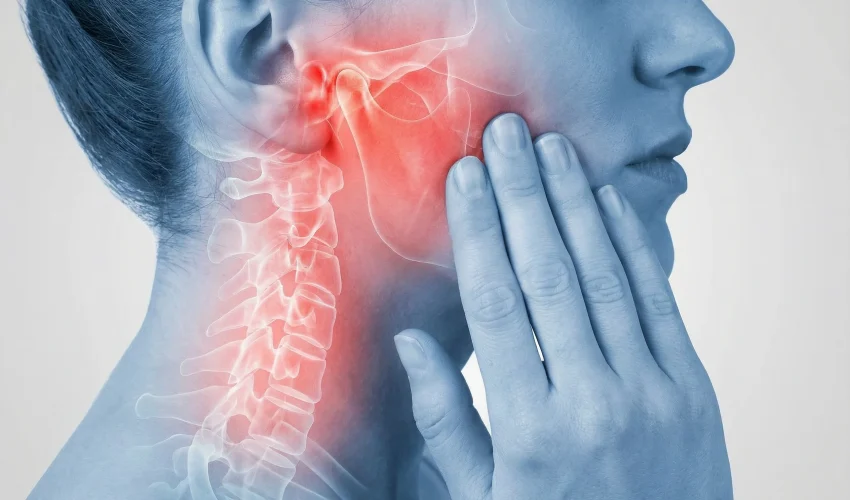
The temporomandibular joint (TMJ) is a small joint located on each side of the face, just in front of the ears. It connects the jaw to the skull and allows movements required for eating, chewing, talking, yawning, and breathing.
When the TMJ or the muscles controlling jaw movement become irritated, inflamed, or sensitive, this can lead to pain, restricted movement, and difficulty with daily activities.
TMJ pain and TMD are often used interchangeably, but they are not the same.
When pain is more widespread around the jaw or affects how the joint functions normally, it is commonly referred to as TMD.
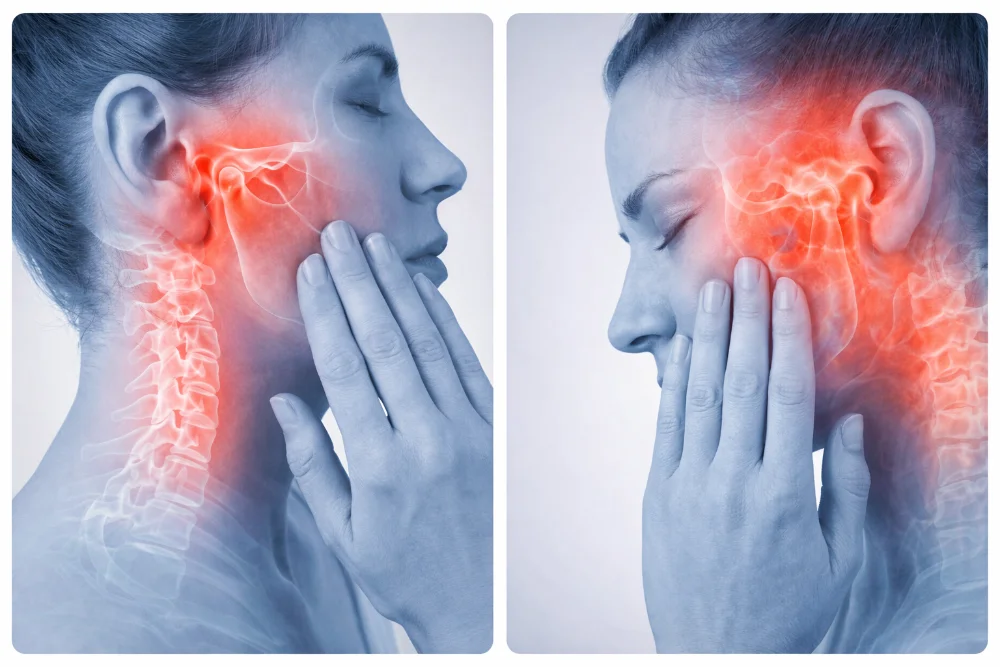
Symptoms can vary in presentation and intensity and may include:
TMJ pain and dysfunction are often influenced by multiple factors rather than a single cause. These may include:
Understanding contributing factors is key to effective management.
If jaw pain or dysfunction is affecting your daily life, a physiotherapy assessment can help determine contributing factors and guide appropriate treatment.
Your physiotherapist will:
Physiotherapy aims to reduce pain, improve jaw function, and support long-term self-management.
Your physiotherapist will help you understand your condition, identify contributing factors, and develop a tailored treatment plan. Where appropriate, treatment may include:
Long-term self-management strategies are an important part of treatment, helping reduce recurrence and improve confidence in jaw movement.
Our physio-led classes are small and often booked out by existing patients. Join the waitlist and we’ll let you know when a spot becomes available or call us to check availability.
We’re now welcoming patients at Pier Street Medical, right next to HBF Park.